Joint replacements to treat painful arthritis of the thumb
- 23 April 2023
- Posted by: invicta_ortho
- Category: Hands
Osteoarthritis affecting the joint at the base of the thumb, known as the 1st carpometacarpal or trapeziometacarpal joint is very common. It may cause pain, particularly with gripping and twisting movements such as opening jars or with any activity which involves applying pressure with the thumb, and if severe even pain at rest. Initially the pain is manged by using your hand differently, pain killers and splints. Beyond this a steroid injection into the joint can relieve the pain, but it’s unpredictable as to how well and for how long.
If the pain remains severe and is affecting someone’s quality of life there are surgical options. The standard surgical treatment for many years has been a trapeziectomy, which involves removing the arthritic bone. Information on this procedure can be found at www.invictaorthopaedics.com. This operation works well in the majority of patients, but recovery of hand function can take several months, and some patients will have persisting symptoms to some degree. Over the years many alternative operations have been tried, including a variety of joint replacements. Unfortunately, most of these had an unacceptably high failure rate and didn’t offer any clinical benefit compared with a trapeziectomy, so I didn’t offer them as an option to my patients. However, there is now good long term follow up data coming out for the new generation of implants. The MAIA prosthesis was first used in 2005, with a dual mobility bearing option introduced in 2015. It consists of a hemispherical cup inserted into the trapezium, a modular neck and an anatomical metacarpal stem. Its fixation is cementless, with a hydroxyapatite coating which encourages bonding to the bone. (Figure 1)
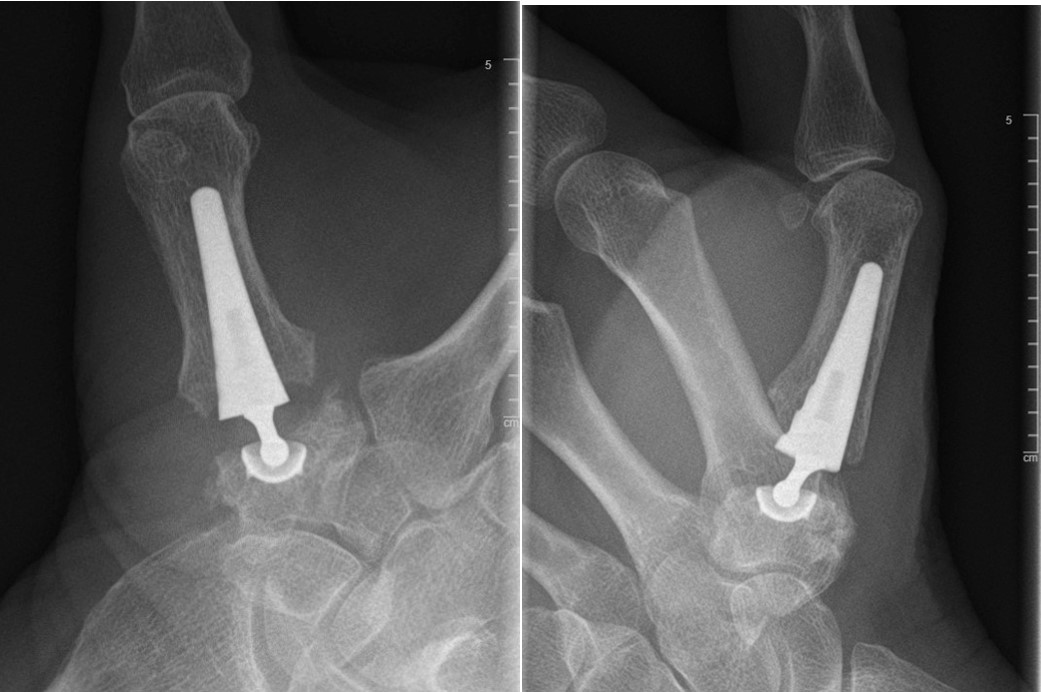
Figure 1
A recent study published in the journal of hand surgery reviewed 191 MAIA prostheses and reported that at the final follow up of 12 years the survival rate of the implant was 88%. The benefits compared with a trapeziectomy are that patients don’t need to go into a plaster cast after the operation, the hand recovers more quickly, and patients who have had a trapeziectomy in one hand and a replacement in the other report that the hand with the replacement feels more normal. On this basis I have started offering a joint replacement with the MAIA prosthesis to my patients. It is not suitable for all patients with painful arthritis at the base of their thumb. If the neighbouring joint is arthritic, or the bone very deformed or weakened by the arthritis a joint replacement isn’t appropriate.
The surgery is done as a day case under an awake regional block or general anaesthetic. Patients don’t need a plaster cast or splint afterwards. There is a bulky bandage for 48 hours, and the wound has to be kept dry until the stitches are removed after 2 weeks. Patients are encouraged to move their thumb straight away and to return to their usual activities over the first month.
Like all operations there are potential complications including infection, dislocation of the ball from the socket and loosening of the implant in the bone. If these complications occur the treatment is to remove the implant and perform a trapeziectomy.
The patients I have treated so far seem to be very pleased with their results, with good pain relief and rapid return to their normal activities. One patient who had arthritis in both thumbs was happy enough with his replacement in one hand to ask to have the same again in his other hand.
If you have painful arthritis at the base of your thumb which has not responded to conservative treatment and would like to discuss surgical treatment please ask your GP for a referral.
Mr JAMES EDWARD NICHOLL

Consultant Orthopaedic Hand, Wrist and Elbow surgery MBBS FRCS (Tr.& Orth.)
